How do you do a Caesarean section? When do you do it? Will they put me to sleep? Could there be complications – and what are they? How will I feel after it? In how long will I “come back to myself” and what will happen in the next pregnancies? The complete guide for the mother
Caesarean section is a means of removing the baby and the placenta through an incision made in the abdomen and uterus. It can be planned or urgent.
A routine surgery takes between half an hour to an hour. At the end, you will be transferred to the recovery room next to the operating room, where you will stay for about two hours.
You can return to normal sexual activity within 4-6 weeks after surgery, but it is advisable to do so after a review and examination by a gynaecologist.
What is a caesarean section?
Caesarean section is a means of removing the baby and the placenta through an incision made in the abdomen and uterus.
A caesarean section can be planned in advance (elective section) – if a problem has been identified(big baby, narrow vaginal passage etc) in advance that requires it or if the woman is interested in it for various reasons; And it can be unplanned (urgent or emergency caesarean) – if a problem arises before or during the birth process.
In the western world, the rate of caesarean sections has increased significantly in the last two decades. In India there has been a relatively moderate increase over the years, and today the rate of caesarean sections is about 18% of births (as of 2016). In the USA, for comparison, the rate of caesarean sections in 2017 was 32%.
Caesarean section may be complex and involve quite a few risks and complications. Since there is no proof that it is better than a normal birth, then when there is no medical directive to perform it, the International Federation of Obstetricians and Gynecologists recommends not to respond to women’s requests to give birth by caesarean section for reasons of convenience.
When is a caesarean section performed?
The reasons that require a caesarean section can be divided into two groups: conditions related to the mother and conditions related to the fetus.
The main reasons related to the mother to perform a caesarean section
Previous caesarean section
This is one of the most common reasons for repeat caesarean section. In general, about half of the women after one previous caesarean section gave birth by caesarean section in the subsequent birth. One of the reasons for this is that attempting a vaginal birth after Caesarean section involves a certain increase in the rate of complications.
Normal birth after caesarean section
The chances of success in a normal delivery after a previous caesarean section depend on several factors, including: the reason for the previous caesarean section; the period of time that has passed since the previous operation (preferably at least a year and a half); has the woman previously given birth in a normal birth; assessing the weight of the fetus and the number of fetuses.
In general, about 75% of women who attempt a vaginal birth after a previous caesarean section succeed.
In any case, it is recommended that any woman who becomes pregnant after giving birth by caesarean section receive personal counseling regarding how it is better for her to give birth in the second birth.
The recommendation for a pre-planned repeat caesarean section exists when: there have been two or more caesarean sections in the past; Estimated fetal weight over 4,500 grams; There was a uterine rupture in the past or the cut on the surface of the uterus in the previous caesarean section was a longitudinal cut in the lower segment; or a cut in the body of the uterus.
Lack of progress in the birth process
If during the birth it turns out that it is not progressing as expected – and it doesn’t matter if it started spontaneously or following a deliberate activation ( induction of birth ) – it is terminated by caesarean section.
Placental position
When the placenta partially or fully blocks the cervix, or it reaches very close to the internal opening of the cervix, it is not possible to give birth in a vaginal birth and caesarean section is the only option. However, even if it turns out that there is a situation of a placenta close to the opening in the early stages of pregnancy, this does not mean that this will also be the case near birth.
Women who are diagnosed with placenta previa usually give birth before completing 37 full weeks – usually due to bleeding. If a pregnant woman is diagnosed with a placental abruption, doctors usually recommend a caesarean section to prevent the possibility of labor and delivery.
Premature separation of the placenta
Placental abruption is a complication of pregnancy in which the placenta separates from the uterine wall before the newborn is born. This complication is not common, relatively, but is more common among women who suffer from chronic hypertension or preeclampsia, as well as among women who smoke and women who have previously suffered from premature separation of the placenta. Abdominal trauma is also a significant risk factor for this complication.
The caesarean sections performed due to placental abruption are urgent operations, and sometimes a blood transfusion is necessary for the mother and the fetus due to the bleeding inside the uterus.
Herpes
Vaginal herpes sores can cause the baby to become infected with the virus. This is a dangerous situation, since the herpes virus can cause various damages to the newborn, including damage to the nerves and eyes and various developmental problems.
That is why it is necessary to check the presence of herpes lesions in the birth canal of every mother who is known to be a carrier of genital herpes. If it turns out that there are indeed herpes sores in the birth canal, it is recommended that the woman be delivered by caesarean section.
Structural defects in the uterus
Women who have structural defects in the uterus are forced in many cases to give birth by caesarean section. The reason: the fetus is often found in their uterus in positions that are not suitable for a normal birth.
However, if the fetus is in a cephalic presentation, a structural defect in the uterus does not necessarily require a caesarean delivery – even if you have given birth once before by caesarean section.
Failure to deliver using devices
Sometimes there is a need to deliver the baby using devices – vacuum delivery or forceps delivery. An attempt to give birth using instruments may sometimes fail, and then it is necessary to do a caesarean section immediately.
The main reasons related to the fetus to perform a caesarean section
Suspected fetal distress
When the monitoring of the fetus suggests that there is a possibility that he is in distress or there is a risk that the continuation of the birth process will endanger him, and the conditions do not allow for a quick newborn or birth with instruments, the medical team will prefer to end the birth by caesarean section.
An embryo representation that is not a head representation
Today, it is customary to deliver by caesarean section any fetus that is not in head presentation. However, in some cases it is possible to allow a normal delivery of fetuses that are in a breech presentation. The same is the case with twin pregnancies, when the first fetus is in head position, and the second is not.
In cases where the fetus is not in head position, you can consult the doctor regarding the possibility of trying to do an external inversion of the fetus . If this procedure is successful, it may save the need for surgery. Usually the preferred time to try the inversion is in the 37th week of pregnancy.
Multiple pregnancy
The increase in the rate of multiple pregnancies in recent years has also contributed to the increase in the rate of caesarean sections. There is controversy regarding how to best deliver in these pregnancies. However, when it comes to two twins who are in cephalic presentation, it is recommended to give birth in a normal delivery.
When the first fetus is not in head presentation, it is recommended to give birth by planned caesarean section. When the first fetus is in head position, but the second fetus is not in this position, it is usually given to the child in a normal delivery, but both options (normal delivery or caesarean section) are considered. The recommendation for the woman will be given individually.
Assessment according to which the fetus is of high weight (macrosomia)
Large babies are usually delivered by caesarean section – mainly because of the desire to prevent a condition called “shoulder impingement” which means that the shoulders get stuck in the birth canal after the head emerges. This is an emergency that cannot be predicted in advance and cannot be completely prevented and that may cause significant damage to both the newborn and the mother.
The incidence of failed normal delivery increases as the weight of the fetus is higher. Because of this, it is customary in India to recommend a caesarean delivery to every woman giving birth with an estimated fetal weight of over 4,500 grams.
In women with gestational diabetes or pre-gestational diabetes, the recommendation is for a caesarean section when the fetal weight is estimated to be over 4,250 grams (and some recommend it even over 4,000 grams), although even with a weight estimate of 4,000-4,500 grams, a normal delivery can be allowed after individual counseling and especially according to the woman’s obstetric history.
Prolapse of the umbilical cord
This is an emergency situation, where the umbilical cord emerges before the newborn. The result may be that when the newborn tries to emerge, he will put pressure on the umbilical cord, and the blood supply to it will be damaged – which may sometimes even cause the death of the newborn. This condition requires an immediate caesarean section.
Brief explanation: in a normal situation, the fetus blocks the way in front of the umbilical cord. However, if the fetus is small or is not in a head position or is not properly fixed in the pelvis, the umbilical cord may drop. This condition is more common in repeated births, in cases of multiple amniotic fluid sac and in cases of early water loss.
What preparations should be made for a caesarean section?
A pre-planned caesarean section is usually done after completing at least 38 full weeks and usually in the 39th week of pregnancy. Sometimes you will be asked to come to the hospital the day before the surgery, and sometimes you will be asked to come on the day of the surgery.
The decision on this is made by the medical team according to the time when the surgery is scheduled.
A caesarean section due to an emergency situation is performed according to the usual procedures for performing emergency operations. In this case there is no preparation in advance.
These are the preparations you should make for a pre-planned caesarean section:
Fasting – you must fast for at least 6 hours before surgery. If you are in the hospital the evening before the operation, you will be given a light dinner, and at midnight you will be required to fast completely. If it is an unplanned surgery, the medical team will try to postpone it so that you arrive after fasting for at least 6 hours.
Taking antacids – before the operation you will receive antacid medicine (you will be asked to drink a substance called sodium citrate) to prevent damage to your lungs in the event that during the operation the vomiting reflex is activated, and as a result you will inhale the contents of the stomach (which is very acidic) into the lungs.
Fluid transfusion – before the surgery , you will have blood tests (usually a test to determine the blood type and blood count ), and you will have a fluid transfusion. The infusion is used not only to administer fluids but also to administer anesthetics during surgery (in case the surgery is done under general anesthesia) and medications.
Hair removal – according to the guidelines of the Ministry of Health, it is not necessary to remove hair from the surgical area, but in some hospitals there is a policy of hair removal in the lower abdomen using an electric shaver. Also remove nail polish, dentures (if any), contact lenses, jewelry, bra and underwear.
Bladder catheter – right before the operation (usually after anesthesia) a catheter (catheter) will be inserted into your bladder. The goal is to empty the bladder to reduce the risk of damaging it during surgery. The catheter is also needed to measure the urine output during the operation and in the first hours after the operation. The amount of urine excreted is used as a measure of blood loss and to diagnose problems with fluid balance (to make sure you don’t become dehydrated). The catheter is usually removed 6 to 12 hours after the operation.
Elastic bandages – Nurse, put elastic bandages on your legs. These are designed to prevent venous thrombosis and are also used to increase blood pressure during surgery. Sometimes instead of using elastic bandages, a special pneumatic device is used that is designed to improve the blood flow in the veins of the legs during and after the operation.
Anesthesia – everything you need to know
What is anesthesia?
Anesthesia is a means of preventing pain during surgery by administering substances that lower the pain threshold, relax and paralyze muscle movement. In this way, it is guaranteed that you will not feel any pain during the operation.
What method will they put me to sleep?
Caesarean section can be done under general anesthesia or regional anesthesia (epidural or spinal). Regional anesthesia is usually preferred, as it is less dangerous for the mother and baby than general anesthesia.
Regional anesthesia has other advantages and one of the most important is that you stay awake and participate in the birth of your baby. The fact that you see and hear the baby and even make physical contact with him at the moment of birth and not just after a few hours is very important for creating the initial connection between you and him.
However, regional anesthesia is not suitable for all mothers. You will make the decision on which type of anesthesia to choose together with the anesthesiologist.
General anesthesia is faster than regional anesthesia, so general anesthesia is suitable in emergency situations (unless you are already under epidural anesthesia), for example when there is severe bleeding or when there is a suspicion that the fetus is in distress.
What should I tell the anesthesiologist before anesthesia?
You must tell the anesthesiologist every important detail of your medical history – about illnesses and surgeries you’ve had in the past, about medications you’re taking and any sensitivity you have to medications.
Will I meet with the anesthesiologist before the caesarean section?
Yes. Before the operation, the anesthetist will examine you. This is the time to ask him about any topic that bothers you about anesthesia. Many people are afraid of anesthesia for surgery. The anesthesiologist will be able to answer any questions you may have about this.
What will they do to me in a caesarean section?
Before the operation, the surgeon will wash the operation area with a disinfectant. A catheter will then be inserted into your bladder and covered with sterile sheets. At the beginning of the operation, the doctors will make an incision in the abdomen through which the baby will be taken out.
The incision is usually made laterally in the lower abdomen (bikini line), but rarely and in specific cases only, the doctors may choose to make an incision along the midline in the lower abdomen. If there is a scar from a previous caesarean section, the doctors prefer to make the incision in the scar itself.
After opening the abdomen, the surgeon makes an incision in the uterus. The incision on the uterus is usually transverse in the lower area of the uterus.
Its advantages: it is easy to sew, it bleeds less, causes less adhesions in the area and is more resistant than all other types of cuts to the risk of tearing during a future vaginal delivery.
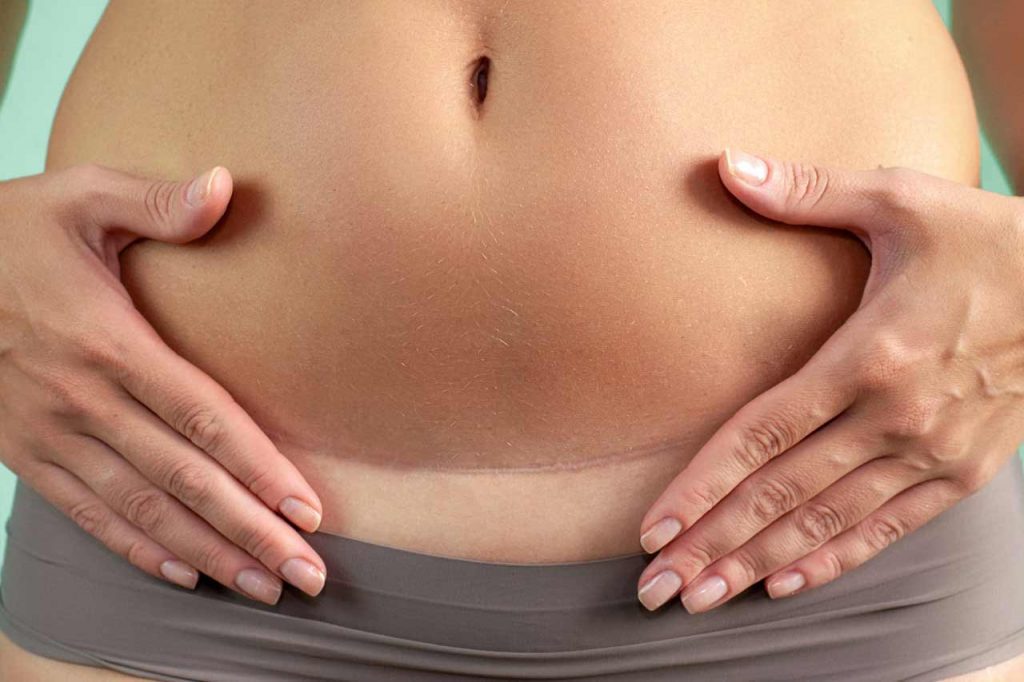
A scar in the stages of recovery from a caesarean section
Another option is to make a longitudinal incision in the uterus (also called a “classic incision”). This incision is mainly used when there is difficulty in extracting the baby or when it is an urgent operation when the pregnancy is still relatively young and the uterus is smaller.
The risk of rupture of the scar area in a longitudinal section is higher than in a transverse section, so doctors recommend that all births after this operation be by caesarean section.
It should be noted that the type of incision in the abdomen does not necessarily correspond to the incision in the uterus.
After the incision in the uterus is completed, the baby is extracted. If it is a lower cut, the leading part is removed first – the head, the buttocks or the legs – and at the same time pressure is applied to the upper part of the uterus.
After the baby is removed, the placenta is removed, making sure that there are no remnants left in the uterus, and then the incisions are closed – first the incision in the uterus and then the incision in the abdomen. The incision on the skin can be closed with staples or with a subcutaneous suture.
How long does a caesarean section last?
A routine caesarean section takes between half an hour and an hour.
How will I feel after the operation and what to expect?
At the end of the operation, you will be transferred to the recovery room next to the operating room, where you will stay for about two hours. If there are no special problems, you will then be transferred to the maternity ward.
After the operation it is very important to get out of bed as early as possible to avoid venous thrombosis – a relatively common complication following the operation. Between 6 and 12 hours after the operation, the catheter is removed from the bladder, and a nurse will help you get off the bed and into the chair. The day after the surgery you can take a shower, and it is very important that you walk around the ward as much as possible.
Sometimes, and depending on the department’s policy and your risk factors for the formation of venous thrombosis, you may be given a subcutaneous injection once a day to thin the blood to prevent the complication of venous thrombosis.
These are the main feelings you will have to deal with immediately after the operation (or after you wake up, in case it is an operation done under general anesthesia).
The first hours after surgery
Pain – after the operation, there may be pain in the area of the operation as well as as a result of the contraction of the uterus. You must report this to the nurse, and she will give you painkillers according to departmental protocols.
Nausea and vomiting – many mothers complain of nausea and vomiting after caesarean section. This can be overcome with a drug that will be given through the infusion.
Dry mouth – in the first hours after surgery you must remain fasting. As a result, you may feel a dry mouth. You can moisten the lips and tongue with gauze soaked in water, but you will receive the fluids in the first hours after the operation only through the infusion. The catheter will also continue to be connected to your bladder, through which you will urinate.
Between 6 and 12 hours after the operation you can drink – but only water and tea. You should avoid drinks that create gas in the digestive system, such as juices and fizzy drinks. You can have food only 12 hours after the operation, and it must be very soft. You will have to make do with foods such as porridge, white cheese, milk delicacies, steamed vegetables and soup. Only after two or three days will you be able to return to normal food.
Restriction of movement – between 6 and 12 hours after surgery (depending on the department’s policy) you will be allowed to get out of bed and take your first steps. The first descent from the bed after the operation will be done with the help of a nurse and will involve pain. Therefore, before getting out of bed for the first time, you can get a pain reliever. Before getting out of bed, the surgical bandage will be removed, and the scar will remain exposed.
The first and second day after surgery
Pain – it is likely that you will also feel pain in the days after surgery, but it is important to prevent them with painkillers. When you are free from pain, you are more relaxed, and your recovery is faster.
Vaginal bleeding – Vaginal bleeding is the result of the uterus being cleansed of the lining that thrived during pregnancy. This lining is secreted with the help of uterine contractions. It is important that you monitor the amount and color of the bleeding. In any case of increased bleeding or bleeding of a cloudy color or bleeding that gives off a bad smell – contact a nurse or doctor.
At first the bleeding is profuse, relatively red in color. After a while the amount decreases, and the color of the bleeding becomes pinkish. Later on, the color of the discharge gradually becomes lighter and lighter. The bleeding lasted a total of up to a month after the birth.
Constipation – if you have not had bowel movements for two to three days after the operation, you can ask the nurse for glycerine suppositories or even a small enema to “restart” bowel activity and put an end to constipation .
Disconnecting the catheter and the infusion system – between 6 and 12 hours after the operation, a nurse will remove the catheter from your bladder and disconnect you from the fluid infusion system.
Movement – it is advisable that you get out of bed as often as possible to ventilate the lungs and stimulate blood circulation.
Hygiene – a nurse will help you shower for the first time. It is important that you wash the surgical area and genitals daily. This can be done with regular soap.
Breastfeeding – due to the many benefits of breastfeeding, it is recommended that you start breastfeeding your baby as soon as possible after surgery. In most cases, you will be able to start breastfeeding close to your return to the ward, just like a mother who gave birth in a normal delivery.
However, despite the great benefits of breastfeeding, it is your right to choose the form of feeding that is right for you. If you have decided not to breastfeed, you must inform the nurse in the neonatal and maternity departments so that they can prepare bottle food for your baby.
Hospitalization time – if no special problems arise, the stay in the maternity ward usually lasts between four and five days (depending on the department’s policy).
The staples or sutures of the operation are usually removed before discharge, on the fifth day after the operation, or in the clinic around the seventh or eighth day after the operation (depending on the policy used in the department). Removing the pins is usually not painful.
What are the possible complications of the surgery?
Caesarean section is relatively safe, and the rate of complications following it is low. However, as with any operation, there may be complications in a Caesarean section. In general, the rate of complications is lower in a first Caesarean section and a preplanned Caesarean section than in repeat Caesarean sections or urgent Caesarean sections.
Before the operation, you will be required to sign a consent form for Caesarean section in which the possible complications are explained. Complications are divided into anesthesia complications, complications during surgery and complications after surgery. Here are the main complications of Caesarean section:
Mortality – Mortality rates as a result of caesarean section are tiny, but still three to four times greater than vaginal birth.
Rupture or expansion of the surgical incision in the uterus – during the operation, a tear may form in the uterus or the surgical incision in the uterus may spread and expand.
Such an entanglement can cause bleeding from large blood vessels of the uterus – a phenomenon that requires the giving of blood doses to the mother, and rarely may even require excision of the uterus to control the source of the bleeding.
Injury to the abdominal organs – injuries to the bladder, ureter or intestines are possible complications of Caesarean section, and especially of repeated Caesarean sections. These injuries are usually identified during surgery and treated immediately with corrective surgery.
Heavy bleeding – on average, a woman in labor loses up to 1,000 cc of blood during a caesarean section. Sometimes the woman in labor bleeds during the operation in a way that endangers her life.
When all efforts to stop the bleeding fail, the surgeon will consider cutting out the uterus in an attempt to save the mother’s life. It should be emphasized that this is a relatively rare complication. It is created mainly in cases where the placenta is embedded in the uterus or there is a tear in the uterus.
Damage to the fetus – this complication is also rare, but it must be taken into account. The injury to the fetus may be caused during the surgical opening of the uterus or during a difficult extraction of the fetus from the uterus.
Infection – fever, uterine or pelvic infection, urinary tract infection or surgical wound infection are the most common complications among women who have had a Caesarean section.
The treatment of infection in the pelvis, uterus or urinary tract is with antibiotics. On rare occasions, relatively, the surgical wound may become contaminated to such an extent that it will be necessary to open it and drain it.
However, most of the operated women will recover quickly after giving antibiotic treatment. Only a few require prolonged hospitalization due to the infection, during which they receive intensive antibiotic treatment.
Thrombosis in the deep veins in the legs and pulmonary embolism – these are relatively rare complications, but can be life-threatening.
The fact that the mother does not move during and after the operation increases the risk of thrombus formation in the veins of the legs and embolism in the lungs – especially during the recovery period from the operation.
Some women are at an increased risk of pulmonary embolism following surgery, and they may receive blood thinning medication after surgery. The drug is given by injection under the skin.
Complications of anesthesia – with any anesthesia there is a risk of complications and side effects.
Will I have restrictions after a Caesarean section?
After Caesarean section, feelings of fatigue, pain, discomfort and weakness. That is why it is recommended that you get plenty of rest and avoid activities that involve effort. It is important that you help family members in carrying out daily activities and chores.
The things you must be careful about when you return home after a caesarean section:
Limitation of effort – for the first three weeks after the operation, make sure to rest. You must avoid overexertion such as lifting heavy loads so as not to damage the surgical incision.
Hygiene – continue to wash the surgical wound with running water to maintain hygiene and monitor the development of signs of infection: redness around the surgical scar, discharge from the surgical scar or vaginal discharge with a smell, body temperature rising to 38 degrees Celsius and more.
Pain – the pain can continue even during the recovery period at home. It is recommended to use painkillers as needed. When the body is free from pain, recovery is faster. You can continue to breastfeed even if you are taking painkillers.
Postpartum bleeding – in the first days after delivery, the vaginal bleeding will be profuse, dark red in color. Later it will turn pinkish to yellowish-white and last for about three to four weeks.
Do not use tampons during this period. Pay attention to the amount of discharge and the smell. If there is increased bleeding (the sign: when more than two pads are changed in half an hour) or if there is a foul-smelling discharge, contact the attending physician or the women’s emergency hospital immediately.
Hemorrhoids – Hemorrhoids bother many mothers – not only those who gave birth by caesarean section – and require great attention to hygiene. You can treat with local ointments that relieve the pain. Within two to three weeks, the local swelling goes down, and the hemorrhoids converge inside – usually without further intervention.
It is important to have daily bowel movements. To this end, constipation must be prevented by drinking a lot and eating fruits and vegetables with the peel. You can use natural remedies to encourage bowel movements. If the problem is not resolved, contact the attending physician.
Weight loss – immediately after birth, mothers lose between four and six kilograms (the weight of the baby, the water and the placenta). After that, the weight loss is very gradual – which frustrates mothers who in many cases gain quite a few kilograms during pregnancy.
It is not recommended to do drastic slimming diets during this period – especially if you are breastfeeding. You can use a dietician to lose weight in a healthy and safe way.
Anemia – Many women suffer from anemia after giving birth, especially if they did not take iron pills during pregnancy. It is recommended to take iron pills from the third day after the operation – and in the same dose that you took (or are required to take) during pregnancy – and to persist in this for six weeks or according to the doctor’s instructions.
Edemas – Edemas appear already during pregnancy and sometimes immediately after birth. This is a physiological condition that passes by itself within five to six weeks after birth. To help yourself, make sure not to wear tight shoes and don’t wear tight jewelry, especially rings. While resting you can place your feet on a pillow.
Changes in mood – after giving birth, you may feel changes in mood or emotional instability that will cause you to cry outbursts. This condition is related to hormonal changes after childbirth. It’s okay – and it passes. The frequency of these symptoms can be reduced with the help of close family members and help in caring for the newborn.
If you have sleep disturbances or anxiety , false thoughts and aggressive impulses – please contact a nurse or doctor immediately, and they will provide you with professional help or refer you to a place where you can receive such help.
It is important to remember that postpartum depression is a recognized and transient phenomenon and not a mental illness. With appropriate help and support the symptoms decrease and disappear.
Sex life – it is possible to return to normal sexual activity within four to six weeks after the operation, but it is advisable to do this after a review and examination by a gynecologist.
It is important for you to know: it is possible to ovulate even before the appearance of the first period, so if you return to having sex without using contraceptives, you may find yourself pregnant again.
When will I “come back to myself”?
in about six weeks.
How long should you wait before getting pregnant again?
For optimal obstetric results and to increase the chance of success in a normal birth in the next pregnancy after the caesarean section, it is recommended that at least a year and a half pass between births.
What rights do I have after a caesarean section?
You are entitled to maternity leave like any other mother.










Add Comment