Breast cancer is the most common cancer in women in the world – one in eight is expected to get it during her lifetime. What causes him? What are his symptoms? What diagnostic tests are available? What are the chances of recovery? Our expert answers
The name of the diagnosis: Carcinoma of the Breast, Breast Carcinoma, Breast Cancer, Ca of Breast
The name of the diagnosis in the doctor’s computer system (CLIX): Malignant Neoplasm of Breast
What is breast cancer?
Breast cancer is a malignant tumor that originates in the breast tissue. It is the most common malignant tumor in women. There are several types of breast cancer, but in all types early diagnosis is crucial.
General explanation: Cancer is formed when one of the cells in the tissue does not stop dividing: it divides repeatedly without control and creates many cancer cells in one area. This concentration of cancer cells forms a mass that can later cause the destruction of nearby healthy tissues and send metastases to distant organs.
In this way, breast cancer spreads to the lymph nodes in the armpits and may metastasize to other organs such as the lungs, bones, and liver.
Early detection and treatment, using the methods detailed below, greatly increase the chances of recovery from the disease.
Breast cancer in numbers breast cancer is the most common cancer among women in the world: one in eight women is expected to get it during her lifetime. According to the most recent information, 1,042 women in Israel died of invasive breast cancer in 2018 (about 14% of those who died – 146 women – were under the age of 50). In the same year, 5,539 new patients were diagnosed with breast tumor (most of them 50 years old and older). The good news: 69.2% of them were diagnosed when they were in the early stage of the disease.
What are the symptoms of breast cancer?
The main symptom of breast cancer is a lump in the breast. However, it should be emphasized that not every appearance of a lump in the breast is necessarily a sign of cancer. These are often cysts (fluid pockets) or benign tumors. Therefore, in any case of suspicion of a lump in the breast, it must be examined by a breast surgeon to determine if further tests are necessary.
There are other possible symptoms of breast cancer:
- Changes in the skin on the surface of the breast and in the structure of the breast.
- Bloody discharge from the nipple.
- Sinking of the nipple.
- Changes in the skin of the nipple (for example, peeling off the skin).
- Enlarged lymph nodes in the armpit.
It should be emphasized: in small tumors, there are no complaints and no findings in self-examination, and the tumor is only detected by mammography or breast ultrasound.
Does breast cancer hurt?
Breast pain is usually not a manifestation of breast cancer, but in any case of new complaints that do not go away on their own, you should contact your doctor and be examined.
What are the warning signs that require an immediate visit to the doctor?
- Palpation of a lump in the breast.
- Change in breast shape or size.
- Change in nipple shape.
- Discharge from the nipple.
What causes breast cancer?
A breast tumor is caused by a disruption in the division processes of the cells in the breast tissue. The cause of this disruption is unknown, but several risk factors are known that increase the risk of developing breast cancer.
These are the known risk factors:
- Hereditary tendency (in the doctors’ language: “a family story of breast cancer”).
- Hormone replacement therapy after menopause.
- Obesity.
- The appearance of the first menstruation at an early age and the cessation of menstruation at a relatively late age.
- First pregnancy at a relatively old age (age 30 and over).
- Smoking.
- Excessive consumption of alcohol (more than one serving of alcohol per day. One serving of alcohol for women is, for example, one glass of wine).
- Breast cancer is more common in Northern Europe, the United States than in East Asia and Africa.
- Breast cancer is 100 times more common in women than in men.
- In the past, it was believed that breastfeeding protects against breast cancer, but today we know that breastfeeding only reduces the risk of getting the disease to a very moderate extent. Because of this misinformation, there have been cases of women who felt a lump in their breasts while breastfeeding and did not get tested because they were convinced that they were protected.
How is breast cancer diagnosed?
The diagnosis is made in many cases following the discovery of a lump or other changes in the breast.
The lump can be discovered by the woman herself or the attending physician. However, it must be emphasized again: in many cases, there is no complaint, sensation, or finding, and the only way to diagnose the tumor is with routine imaging tests: mammography or breast ultrasound.
Manual examination
The medical establishment (in this case the National Council on Oncology, Prevention and Early Detection of Cancer) does not currently recommend that medical teams encourage women to do breast self-examination.
The reason: from studies that have been done, it appears that these self-examinations do not usually lead to an early diagnosis and even often result in many invasive investigative actions that in retrospect turn out to have been unnecessary.
However, every woman needs to be aware of her body, and if she notices any change in the appearance of the breast or a new finding, she should seek a doctor’s examination as soon as possible.
doctor’s checkup
It has not been proven that a routine breast examination by a doctor helps in the early diagnosis of breast cancer.
Nevertheless, it is advisable to be examined from time to time by a doctor specializing in breast examinations to assess the risk of contracting the disease (based on age, family history, and other risk factors) and to receive individual recommendations regarding routine follow-up for early diagnosis. The recommendations are adapted to age and risk level.
Mammography
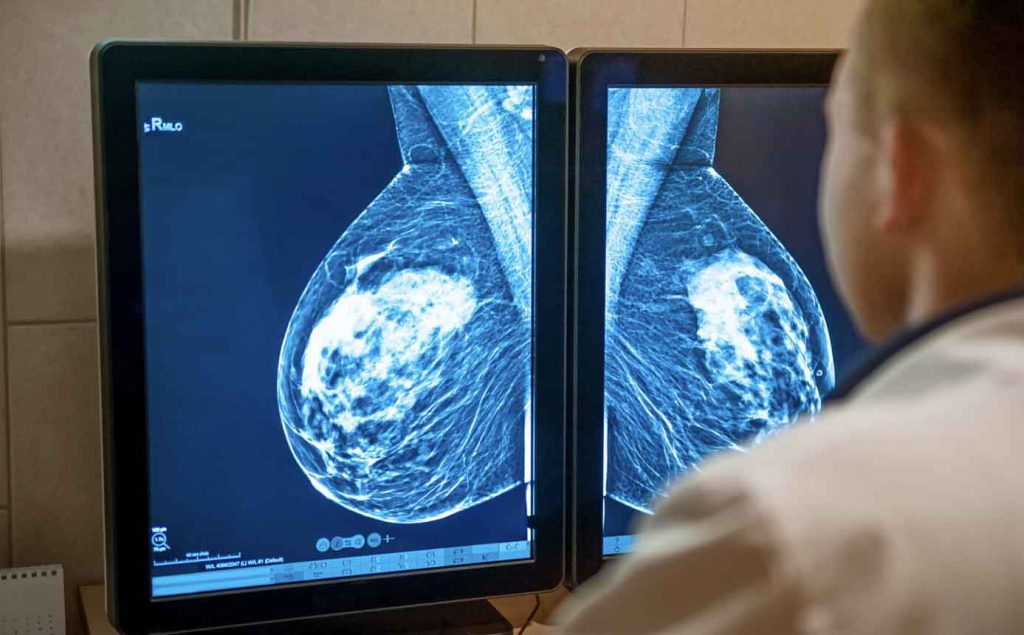
Mammography ( x-ray of the breast) is the best and most widely used test for early diagnosis of breast cancer.
Mammography makes it possible to discover small lumps that cannot be felt through palpation. Detecting the tumor at an early stage significantly reduces mortality from breast cancer.
According to the guidelines of the Ministry of Health, it is recommended that every woman have a mammogram once every two years starting at the age of 50. For women who are at increased risk, for example, women who have a first-degree relative who contracted the disease at a young age or women whose families have many cases of breast and/or ovarian cancer, it is recommended to start the follow-up is already at the age of 40 and do it every year.
As mentioned, every woman over the age of 50 is recommended to have a routine mammogram once every two years. For women who are in a risk group (for example, whose families have many cases of breast cancer and/or ovarian cancer) the test is recommended from the age of 40, and it must be done once a year or according to the doctor’s recommendation.
The Association of Surgeons promotes a new approach of personalized screening tests based on the level of risk. For women at normal risk, it is recommended – according to this approach – to have an annual mammogram from age 45 to age 60, and one every two years starting at age 60.
For women at increased risk, it is recommended to “tailor” a follow-up plan that takes into account the risk factors and the structure of the breast (for example, add ultrasound for women with dense breast tissue).
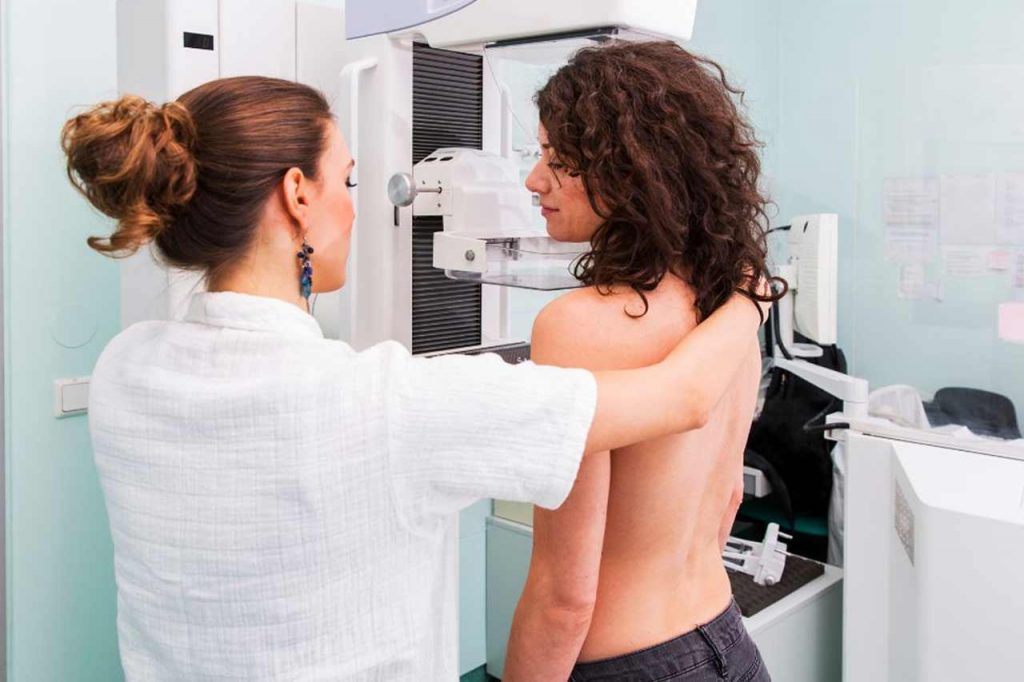
Mammography test
A mammogram is an X-ray of the breasts. This is a non-invasive test that uses low-dose X-rays to create images of breast tissue. In the basic examination, two photographs are taken of each breast.
Mammography is used as a screening test to diagnose breast cancer in its early stage before a lump can be felt on a breast exam.
3D Mammography:
As medical advancements continue to revolutionize the field of healthcare, one significant breakthrough that has revolutionized breast cancer screening is 3D mammography, also known as breast tomosynthesis. This cutting-edge imaging test combines multiple breast X-rays to create a detailed three-dimensional picture of the breast, providing healthcare professionals with a clearer view of breast tissue and enhancing the accuracy of breast cancer detection.
3D mammography offers several advantages over traditional 2D mammograms. For women with dense breast tissue, the 3D image allows doctors to see beyond areas of density, improving breast cancer detection in such cases.
Additional tests after Mammography:
- Breast ultrasound. This is a complementary test to mammography, and can also be used to detect breast tumors. This test is especially important when it comes to women who have dense breast tissue – which limits the effectiveness of mammography. It should be emphasized that a breast ultrasound is not a substitute for a mammogram, since even in women with dense breast tissue there may be findings that are visible in the mammogram and not visible at all in the ultrasound.
- An MRI of the breast is recommended and is in the health basket for women who are at an increased risk of developing breast cancer on a genetic basis – for example, those who have a mutation in the BRCA1 or BRCA2 genes (two genes that cause an increased tendency to get breast cancer). The test is also recommended for those whose families have many cases of breast cancer and/or ovarian cancer or whose medical history includes radiation to the chest wall in childhood.
- Biopsy of the breast. When a suspicious finding is discovered in the breast, it must be checked directly by taking a biopsy. The biopsy can be taken under local anesthesia with a thin needle or with a slightly thicker needle.
In most cases, breast cancer is diagnosed at a stage where it is limited only to the breast and has not yet metastasized to other organs. If metastases are suspected, additional imaging tests such as CT should be done.
What are the types of breast cancer treatment?
Doctors have several means of treating breast cancer:
• Analysis. Women diagnosed with a breast tumor usually undergo surgery to remove the tumor (lumpectomy – partial excision of the breast). They also take a sample from the lymph nodes in the armpit (sentinel gland biopsy).
Sometimes a more extensive operation is necessary: removal of the entire breast (mastectomy – complete excision) and extensive excision of the lymph nodes from the armpit. When it is necessary to perform a complete mastectomy, it is possible – in most cases – to immediately perform surgery to reconstruct the breast.
• Funding. After surgery, there is usually a need for complementary radiation therapy – especially if it was a partial excision. The radiation can be given to the entire breast, and sometimes it is also given to the area of the lymph nodes that drain the breast. In some cases, it is possible to be satisfied with one dose of radiation given during the resection surgery.
A woman undergoes radiation treatments
• Chemotherapy. Chemotherapy includes drugs that damage the tumor cells. The chemotherapy treatment sometimes has side effects such as nausea, vomiting, and hair loss. These side effects can be alleviated with medication. It should be noted that not every case where breast cancer is diagnosed requires the administration of chemotherapy. Chemotherapy can be given before or after surgery.
• Biological treatments. Unlike chemotherapy treatments, biological treatments are more specific to the tumor cells and reduce the damage to the rest of the body’s cells, so they have fewer side effects. Biological drugs that are used against breast cancer are, for example, Herceptin and Lapatinib.
• Antihormonal treatments. After the end of chemotherapy and radiation treatment, it is recommended that some patients receive complementary antihormonal treatment in pills for 5 to 10 years. Such treatment is suitable for women whose tumors had receptors for hormones, and its purpose is to reduce the risk of tumor recurrence. An example of an anti-hormonal drug is tamoxifen.
What are the chances of recovery from breast cancer?
The chances of recovery from breast cancer depend on the type of tumor, its characteristics (for example, whether it is sensitive to hormones or not), the stage at which the diagnosis was made, and the general health of the woman.
In most cases, when there is an early diagnosis, and the woman receives the treatment adapted to the characteristics of her disease, the recovery is expected to be complete. After a few years without the recurrence of the tumor, it can be said that a full recovery from the disease has been achieved. If the tumor recurs, treatments adapted to the characteristics of the disease and the stage of the disease will be recommended again.
It should be noted that survival rates from breast cancer in Israel are among the highest in the West. This figure probably stems, among other things, from the early diagnosis through the screening tests that are customary in Israel and the high response to their performance.
From a publication of the Cancer Society (September 26, 2019) the following facts emerge regarding the survival chances of breast cancer patients:
- There is an increase in the rate of early detection: in 2016, the disease was diagnosed at an early stage in 64% of all new patients. In contrast, in 2005, the disease was diagnosed at an early stage in only 58% of patients.
- Five-year survival rates from breast cancer are relatively high in Israel: 89% among Jewish women and 84% among Arab women. These figures place Israel in 14th place (above average) among the OECD countries.
- A distinct downward trend in mortality from breast cancer was observed in Jewish women at a rate of approximately 2% per year. In the last decade, there has been a decrease of about 25% in mortality rates from breast cancer.
Could there be complications?
Complications may develop both as a result of the tumor and following the treatments.
Complications of the tumor
• Complications in the area of the tumor: the destruction of the breast, ulceration, and damage to the chest wall.
• Complications of the metastases: if there are metastases, the complications vary depending on the location of the metastases. For example, bone metastases can cause severe pain. Lung metastases can cause coughing and breathing difficulties.
Complications of the treatment
• In any operation there may be complications (such as bleeding or infection). However, breast surgeries are relatively simple (there is, for example, no opening of the chest or abdomen), so complications are rare and usually not serious.
• Radiation therapy can cause a burn in the irradiated area, but this goes away with time.
• Chemotherapy can cause, among other things, nausea and vomiting, hair loss, damage to the heart, suppression of the immune system, and anemia. However, the side effects of chemotherapy are mostly reversible after stopping the treatment.
How soon will I “come back to myself”?
The answer to this question depends, of course, on the type of treatment. Many of the women who are diagnosed with breast cancer undergo breast-conserving surgery and radiation and receive anti-hormonal therapy. Those who are treated in this way are expected to return to full function within a few weeks of the operation.
Complementary chemotherapy treatment (if necessary) lasts several months. At the end of these months of treatment, the woman can gradually return to normal life. After several years without recurrence of the tumor, it can be determined that the patient has fully recovered from the disease. Today, most women diagnosed with breast cancer recover completely from their disease.
If the tumor recurs, the physical and emotional challenges are greater. In such a case, the period until full recovery may take longer.
Thanks to the awareness of the disease and the great investment in developing treatments to cure it, there are now many treatment options, and the chances of recovery are higher than in the past. But unfortunately, breast cancer can still be a serious and deadly disease.
How do you learn to live with breast cancer?
Receiving a message about the discovery of breast cancer is always difficult news, and it takes time to digest. It is recommended to use possible support circles: family, friends, members of the medical staff, the Cancer Society, and the “One in Nine” association. If possible, it is important to try to maintain the routine of life as well as learn about the disease and the treatments to know what to expect.
You should know that in every breast center and every oncology institute, there is a medical team that is available to accompany and assist in everything possible. It is important to ask the staff members all the questions that arise and do not hesitate to contact them with any problem.
Complementary medicine treatments can be used, but this must be done in a controlled manner and with the full cooperation of the treating medical team.
In any case, it is recommended to maintain a healthy lifestyle during the treatments and after recovery: avoid smoking and alcohol, adhere to a healthy diet, maintain normal body weight, and persist in moderate physical activity that is adapted to the physical condition.











Add Comment