The symptoms of atopic dermatitis include an itchy rash and dry skin. What does skin asthma look like in babies, children and adults? Does nutrition affect the disease? Is it contagious? How do you treat it? All the answers to the burning questions
Atopic dermatitis (asthma of the skin) is a chronic inflammatory disease of the skin. It usually starts in childhood.
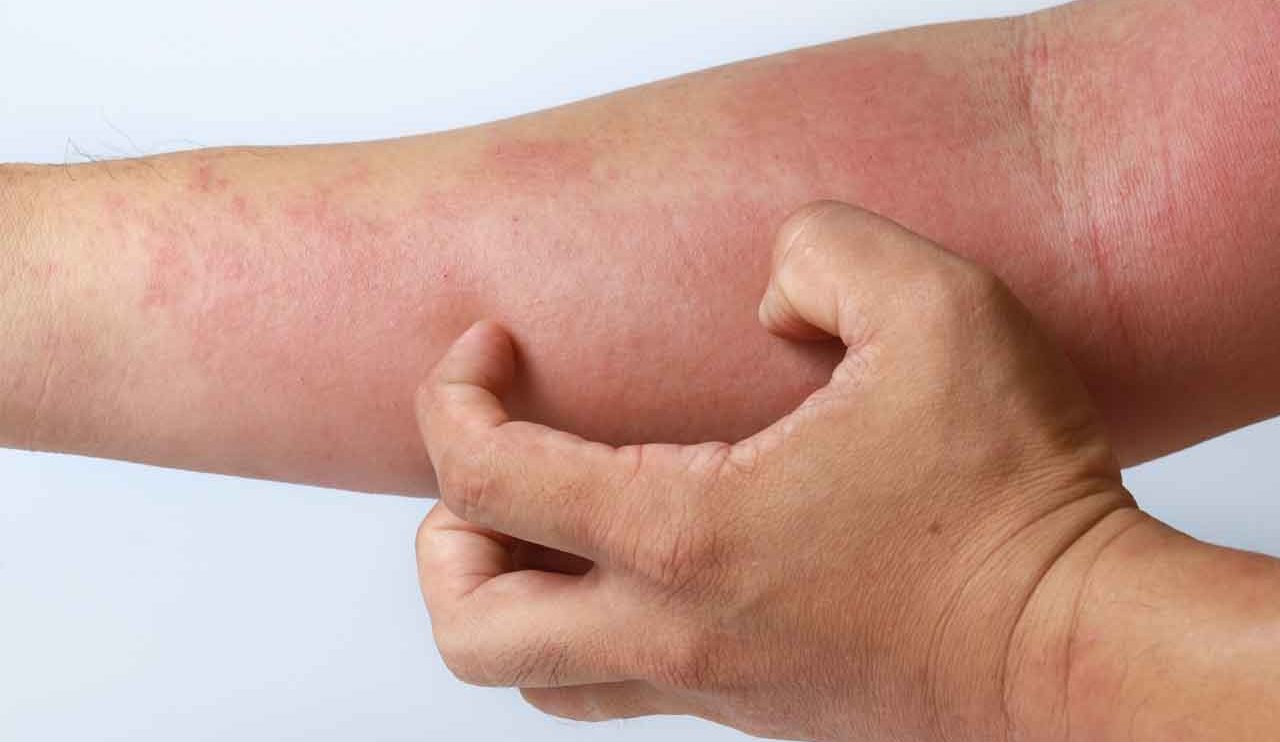
It manifests itself in an itchy rash. Dryness of the skin, irritants and mental stress may worsen the disease.
The treatment of atopic dermatitis includes avoiding skin irritations, keeping the skin moist and sometimes medication.
Doctors call it by its scientific name atopic dermatitis (in English: atopic dermatitis) or atopic skin inflammation. In the general public it is known as asthma of the skin, and some call it atopic eczema.
No matter what you call it, the bottom line is the same: it is a chronic inflammatory disease of the skin that affects about 10% to 20% of all babies and children worldwide, and does not miss some adults either (about 3% to 7% of them).
What does skin asthma look like? What are the symptoms?
Atopic dermatitis manifests itself in the following symptoms:
- Skin rash.
- Significant itching.
- General dryness of the skin.
- In acute attacks, red lesions appear, which are sometimes accompanied by blisters or scabs.
- In prolonged (chronic) conditions, the skin tone is red-brown, it is thickened, and the lines of the skin can be distinguished against the background of its thickening.
The distribution of the disease depends on the age of the patient:
- In cases of atopic dermatitis in babies (starting at two months of age), the rash appears mainly in the areas of the scalp, face and the straightening parts of the limbs (knees and elbows).
- In cases of atopic dermatitis in children (from two years of age onwards), the rash tends to appear in the folds of the body: in the neck, in the hollows of the elbows and knees.
- Cases of atopic dermatitis in adults have a varied clinical expression. On the one hand, there may be a rash in the folds of the body, similar to the situation in children; On the other hand, there may also be an isolated appearance of a rash around the eyelids or on the palms or a widespread appearance in the straightening areas of the limbs (knees and elbows).
Acute lesions of atopic dermatitis that include blisters and scabs
What are the causes of atopic dermatitis and its worsening?
Skin asthma results from a disturbance in the formation of the upper skin layer, in a way that leaves it permeable to various stimuli that create skin inflammation. Therefore, it is not an allergy of the skin to a specific factor, but a general tendency of the skin to react to various factors that penetrate it.
The disease may worsen due to the following factors:
- Dryness of the skin – including use of soap and detergents, prolonged baths, cold and dry weather.
- Irritating substances – wool and synthetic fabrics, exposure to perfumes and care products, dust, sand, grass, pollen of plants and various flowers and mold.
- Mental stress and tension worsen the disease according to various studies.
- The disease tends to worsen in winter when the humidity is lower. However, there are patients who suffer from an aggravation of the disease specifically in the summer when the heat and sweat are evident.
Does nutrition affect atopic dermatitis?
Patients with atopic dermatitis have an increased risk of being sensitive to certain foods.
However, the risk that exposure to these foods will worsen the skin disease is quite rare. In the vast majority of cases, avoiding these foods or other foods does not improve the condition of the skin. That is why you should consult a doctor before deciding to avoid any foods.
Is it an inherited disease?
It is evident that atopic dermatitis has a genetic origin. Many of the patients with the disease have a first degree family member who suffers from atopic dermatitis or from other diseases that are included in the group of allergic diseases such as respiratory asthma , seasonal rhinitis (allergic rhinitis) and allergic conjunctivitis ( spring conjunctivitis ).
In genetic studies, several genes were discovered that a change in them could greatly increase the risk of atopic dermatitis. The most famous garden is called Pilgrimage. A mutation in it (which is very common in the population – 5% to 10% in European populations) increases the risk of atopic dermatitis dozens of times.
How is atopic dermatitis diagnosed?
The diagnosis is based on questioning the patient and a physical examination from which the following supporting findings emerge:
- Itchy rash with typical distribution.
- Prolonged course of illness.
- The onset of the disease in infancy.
- Personal or family history of other allergic diseases (such as respiratory asthma and seasonal rhinitis).
Despite the fact that there are laboratory tests that can support the fact that it is atopic dermatitis (such as measuring the level of IgE antibodies in the blood ), a positive result does not necessarily indicate the disease, and a negative result does not necessarily rule it out.
Is asthma of the skin a disease of children only?
The disease can appear at any age, including adults, but mainly affects babies and small children. In 65% of cases atopic dermatitis appears for the first time already in infancy and in 90% of cases – before the age of 5.
Contrary to convention, atopic dermatitis does not disappear in all children, and 40% of them continue to suffer from it in one form or another even after the age of 12.
A baby who suffers from asthma of the skin on the face and body
What about recovery from atopic dermatitis?
As mentioned, atopic dermatitis mainly characterizes childhood. Studies show that about half of the children will stop suffering from the disease, while half of them will continue to suffer from it even when they are adults.
Both in childhood and in adult life, the disease is characterized by episodes of exacerbations and remissions related, as mentioned, to environmental elements such as the weather, humidity, contact with substances that irritate the skin and an aqueous environment.
Is it a contagious disease?
No, atopic dermatitis is not contagious.
Is she dangerous?
Atopic dermatitis does not endanger the patient’s life, but it is a long-term disease that can significantly affect the quality of life. In extreme situations, where the rash appears all over the body, there is a risk of disturbances in the regulation of body temperature and loss of fluids.
Prolonged lesions of atopic dermatitis include thickening of the skin and a scaly texture
Treatment of atopic dermatitis
The therapeutic approach to atopic dermatitis consists of following a certain lifestyle, regular preventive treatments and treatment when the condition worsens.
• Avoiding skin irritants common to most patients such as tight clothing, woollen clothes, detergents, perfumes and grass.
• Skin lubrication . The most important means of alleviating the disease and avoiding its worsening is keeping the skin moist.
When you shower, you should make sure to bathe in lukewarm water for a short period of time (5 to 7 minutes) with perfume-free soap, which does not dry the skin, or with bath oil. Apply moisturizer immediately after showering.
Many types of moisturizer are marketed. It is recommended to try on a sample before purchasing to ensure a personal fit for the skin, as different people can react differently. It is recommended to avoid natural preparations such as coconut oil and apple cider vinegar since they contain ingredients that may irritate the skin.
Research even shows the possibility that continuous lubrication of the baby’s skin may prevent the development of atopic dermatitis and even other allergic diseases among babies with an increased risk of the disease.
• Treatment of itching . Itching is the most difficult phenomenon in atopic dermatitis, and its treatment is an important step in the treatment of the disease.
Antipruritic drugs from the antihistamine family are a common treatment for atopic dermatitis. However, while these drugs are very effective in treating seasonal rhinitis or allergic conjunctivitis, they are less effective in treating atopic dermatitis.
And what happens if the situation worsens?
In case of worsening of atopic dermatitis, the patient should be examined by a dermatologist, and he will recommend one or more of the following drug treatments:
Topical preparations containing steroids
Such treatment reduces the itching and inflammation associated with outbreaks. There are many preparations (creams and ointments) that contain steroids, so you should consult a doctor regarding the exact preparation, the required dose and the recommended duration of treatment for fear of incorrect use that will lead to side effects. However, this is a safe treatment, and if it is carried out precisely according to the instructions – the risk of side effects is low.
It should be noted that, as a general rule, oral steroid treatment is not acceptable and leads to worsening of the rash shortly after stopping it.
Non-steroidal topical preparations
- Local medications (cream or ointment) containing calcineurin inhibitors can be used for a long time . Their use can also be in areas prone to the development of side effects when other preparations are used (such as eyelids and body folds).
- Staquis (crisaborole). In 2021, a new ointment that is not based on steroids and is based on the inhibition of the phosphodiesterase enzyme entered the medicine basket. The drug is effective in patients suffering from mild to moderate atopic dermatitis. Its great advantage is that it does not contain steroids, so it can be used for a long time in sensitive areas. The use of the drug is from the age of two and more.
Treatment of infection
If necessary, the doctor may decide on parallel treatment of the secondary bacterial infection using antibiotics.
Treatment of moderate to severe chronic atopic dermatitis
In cases of moderate to severe atopic dermatitis that affects large areas of the body, and that cannot be controlled using the drugs mentioned above, or that requires prolonged treatment with local steroids, there are several treatment options:
- Phototherapy . Gradual exposure to UVB radiation in phototherapy centers effectively treats atopic dermatitis. The treatment includes short exposure to radiation (between seconds and a few minutes) several times a week. Often there is a prolonged retreat of the disease following this treatment.
- Immunomodulatory drugs. Medicines such as methotrexate , cyclosporine , imorane and salcept are known for their ability to effectively treat atopic dermatitis. The attending physician is responsible for adjusting the treatment, the dosage and the side effect profile to the patient.
- Dufixant (dufilomb). It is a biological drug consisting of an antibody to the Il-4 receptor, a small protein that mediates a significant part of the activity of atopic dermatitis. The effectiveness of the treatment and its safety are very high. It is given by subcutaneous injection once every two weeks and does not require monitoring through laboratory tests. This drug is indicated in Israel for moderate to severe atopic dermatitis in patients aged 12 years and older after the failure of treatment with immunomodulatory drugs.
- There are new treatments, which are not yet available on the market, using drugs that inhibit the JAK enzyme or that block the IL-13 receptor. In early clinical studies, these drugs have been shown to treat atopic dermatitis very effectively.
When should you see a dermatologist?
If the basic treatment by oiling the skin does not help, and if you need to apply topical steroids for a long time (more than a week a month), you should consult a dermatologist.
What are the warning signs that require an immediate visit to the doctor?
- Sudden aggravation of the skin disease (especially if it is accompanied by high fever).
- The appearance of blisters on the surface of the diseased areas.
- Significant worsening after stopping treatment.











Add Comment